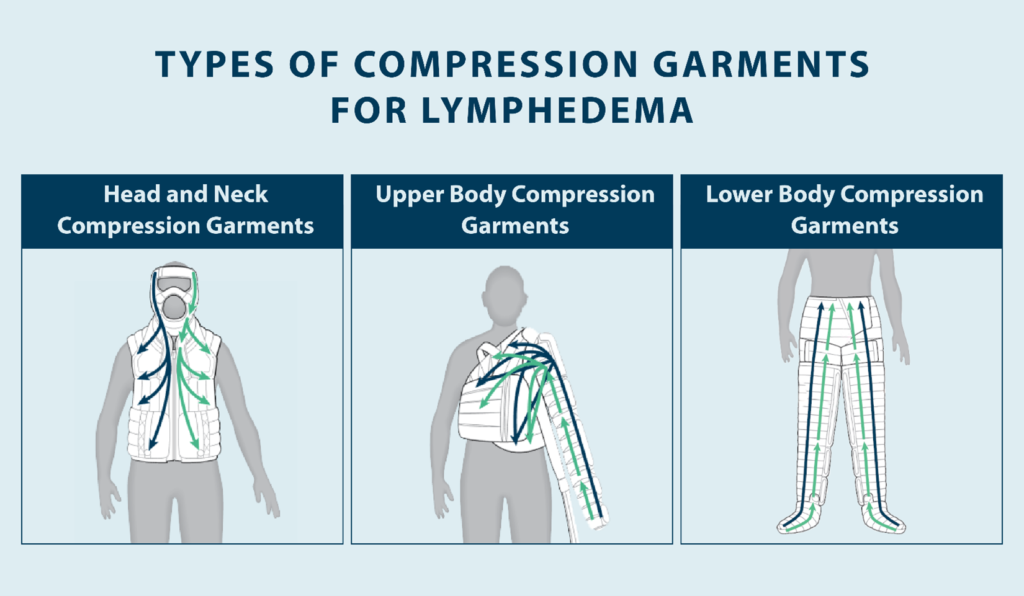
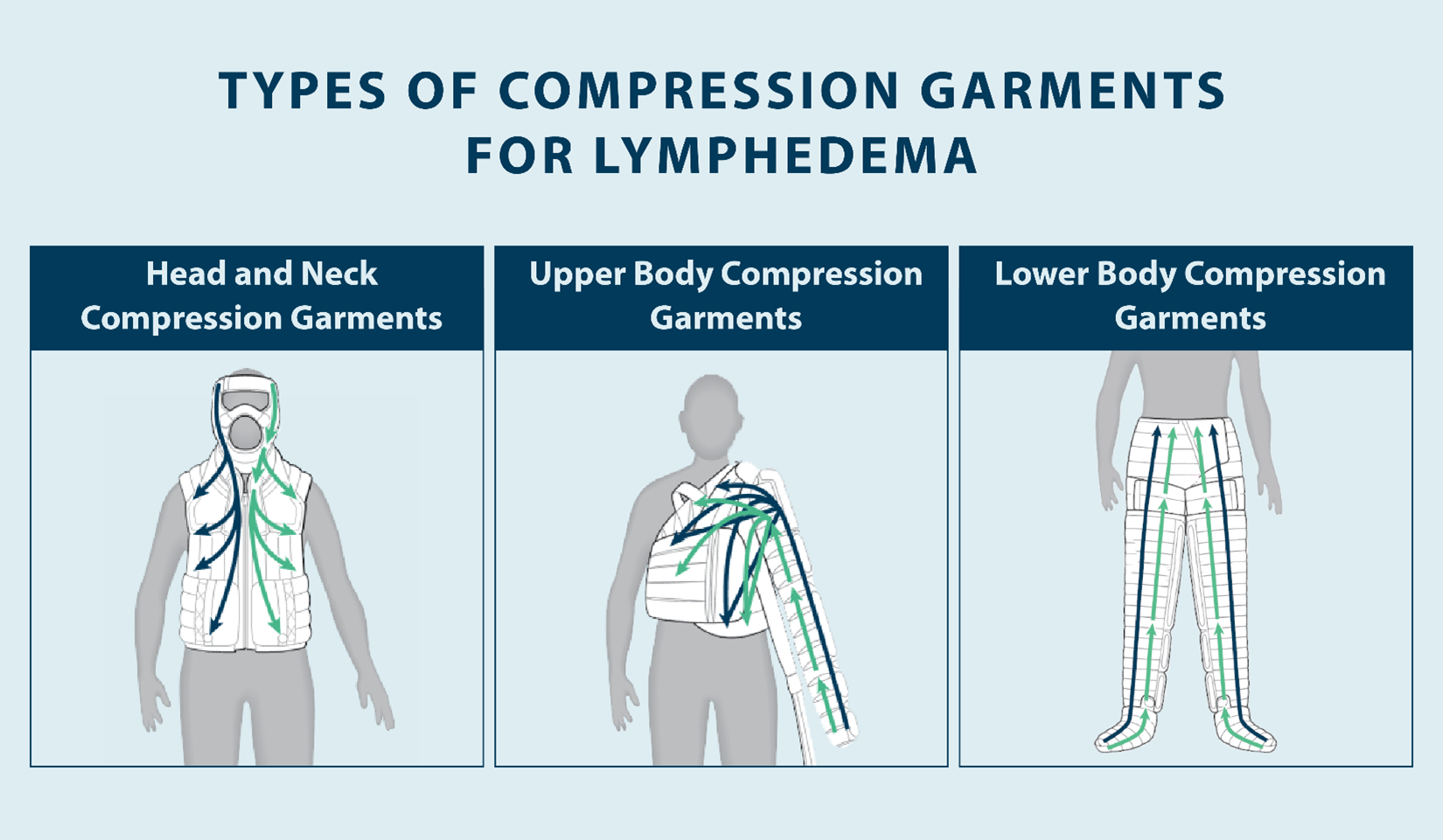
What Is Compression Bandaging?
Compression bandaging is an effective therapeutic technique that uses multiple layers of short stretch bandages to stimulate your lymphatic system to reduce excess fluid and facilitate increased flow and drainage of lymph fluid.

With compression bandaging, you need to have your bandaging applied by a lymphedema specialist at first. However, most therapists will instruct the patient in self gradient compression bandaging so they can apply bandages themselves at home, and many do this every night on their own. Daily bandaging may be part of intensive treatment for lymphedema, and that bandaging may be accompanied by lymphatic drainage massages.
When applying compression bandaging, a specialist will use different types of bandages in multiple layers to create compression on the affected limb. This bandaging may include a soft foam layer, a dense foam layer, and multiple layers of bandaging. Some newer products include both the foam and compression bandaging in one layer, which can reduce the amount of time compression bandaging takes to apply.
Once you’ve had compression bandaging applied, you need to follow therapy instructions when it comes to bathing and showering. If you’re going to take a bath or shower at home, you need to make sure you’re covering up your bandaging. Water can affect the compression these bandages provide and can encourage bacterial growth underneath the bandaging. In some cases, you may be able to take a shower in between compression bandaging applications. If that’s the case, make sure you thoroughly dry and moisturize your skin after you’ve showered but before you have new compression bandaging applied.
Because compression bandaging can be cumbersome, it’s recommended to wear loose fit clothing when bandaged. Your doctor or specialist may provide instructions for exercises you can do to help reduce swelling and stimulate your lymphatic system; make sure you’re doing these exercises on a regular schedule.
You should only apply compression bandaging under the supervision of a lymphedema specialist because without proper training it can be dangerous. There are certain types of bandages that are used for gradient compression. When applied by a specialist, compression bandaging can be an effective form of lymphedema treatment.